

《柳叶刀肿瘤分册》2017年7月4日在线先发
http://thelancet.com/journals/lanonc/article/PIIS1470-2045(17)30441-2/fulltext
脑转移灶切除后行立体定向放射外科治疗与全脑放疗的比较(NCCTG N107C/CEC3试验):一项多中心、随机对照3期试验
背景
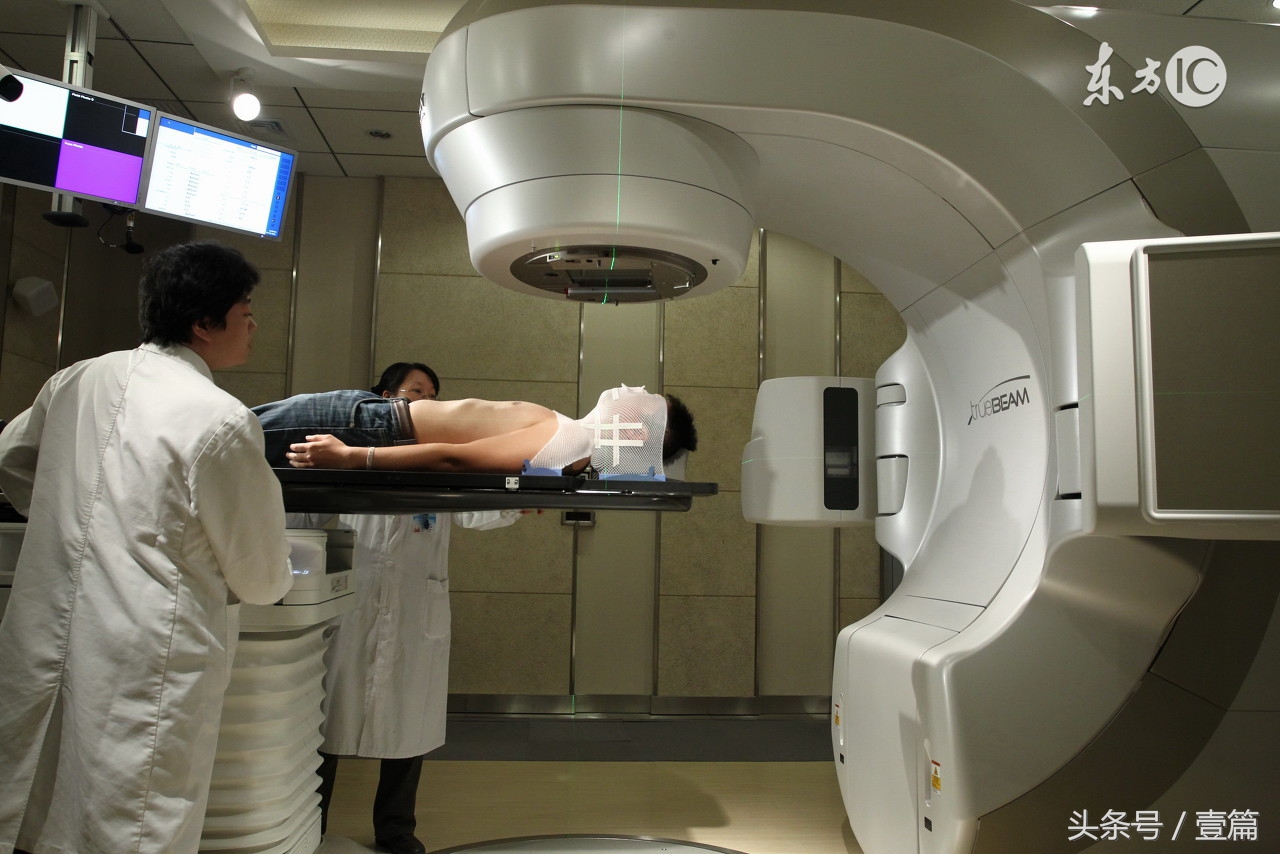
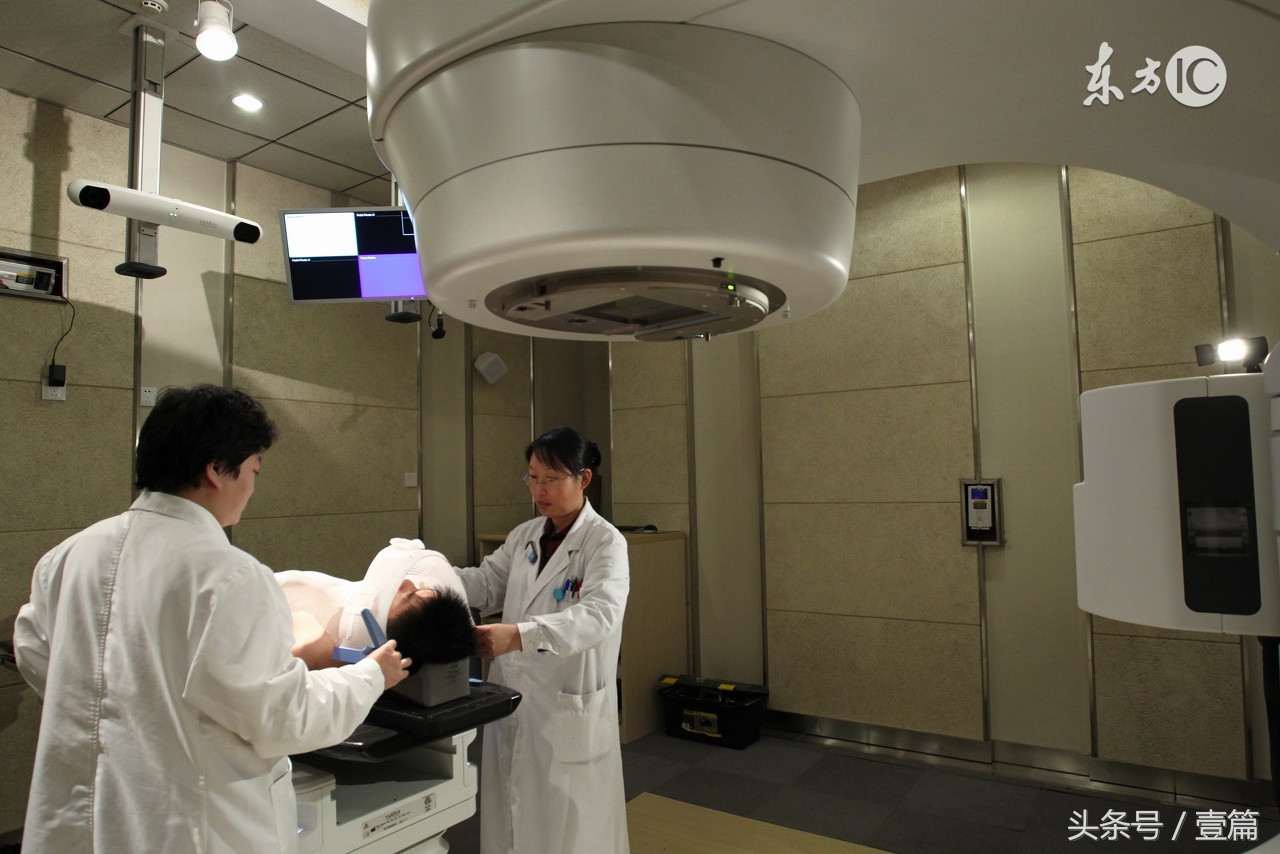
全脑放疗(WBRT)是脑转移灶切除后改善颅内控制的标准治疗,然而,尽管术腔区域立体定向放射外科治疗(SRS)在这种术后情况下的确切疗效尚缺乏高级别的对比性数据,但已广泛使用,以尝试减少对认知的毒性作用。在此,我们在脑转移灶切除的患者中,旨在确立立体定向放射外科治疗与全脑放疗相比,对生存和认知结果的影响。
方法
在这项随机对照3期试验中,将来自美国与加拿大的48家医疗机构、切除了一个脑转移灶且最大术腔范围小于5cm的成年患者(18岁及以上)随机分组(1:1),一组接受术后立体定向放射外科治疗(12-20Gy,单次分割,分割剂量取决于术腔体积),另一组接受全脑放疗(30Gy,分割10天10次,或37.5Gy单次2·5Gy,分割15天15次;在治疗中心为所有患者制定分割计划)。我们使用一个动态分配策略来随机分配患者,并按年龄、颅外肿瘤控制时间、脑转移瘤数目、组织学、最大术腔直径和治疗中心进行分层。患者和研究人员知晓治疗分组。主要复合终点为无认知功能减退生存期和总生存,采用意向性治疗进行分析。我们报告终期分析。这项临床试验在ClinicalTrials.gov注册,注册号NCT01372774。
结果
2011年11月10日至2015年11月16日,入组患者194名,并随机分配到立体定向放射外科治疗组(98名)或全脑放疗组(96名)。中位随访时间11.1个月(IQR,5.1-18.0)。立体定向放射外科治疗组患者的无认知功能减退生存期(中位值3.7个月[95%CI,3.45-5.06],93名患者出现认知功能减退)长于全脑放疗组(中位值3.0个月[2.86-3.25],93名患者出现认知功能减退;风险比[HR]0.47[95%CI,0.35-0.63];p<0.0001),接受立体定向放射外科治疗的患者6个月时认知功能减退发生率低于全脑放疗组(立体定向放射外科治疗组54名可评价患者中有28名[52%],全脑放疗组48名可评价患者中有41名[85%];相差−33.6%[95%CI,−45.3至−21.8],p<0.00031)。立体定向放射外科治疗组中位总生存期12.2个月(95%CI,9.7-16.0,69名死亡)、全脑放疗组11.6个月(9.9-18.0,67名死亡)(HR1.07,95%CI,0.76-1.50;p=0.70)。发生率大于4%的最常见3、4级不良反应为听力障碍(立体定向放射外科治疗组93名患者中有3名[3%],全脑放疗组92名中有8名[9%])和认知障碍(3[3%]对比5[5%])。无治疗相关性死亡。
解释
全脑放疗比立体定向放射外科治疗认知功能下降更易发生,两个治疗组间总生存期无差异。脑转移灶切除后,对于这类患者,应当考虑立体定向放射外科治疗为标准治疗之一,可作为替代全脑放疗、毒性更低的替代方案。
《壹篇》孙莉

Postoperative stereotactic radiosurgery compared with whole brain radiotherapy for resected metastatic brain disease (NCCTG N107C/CEC·3): a multicentre, randomised, controlled, phase 3 trial
DOI: http://dx.doi.org/10.1016/S1470-2045(17)30441-2
Background
Whole brain radiotherapy (WBRT) is the standard of care to improve intracranial control following resection of brain metastasis. However, stereotactic radiosurgery (SRS) to the surgical cavity is widely used in an attempt to reduce cognitive toxicity, despite the absence of high-level comparative data substantiating efficacy in the postoperative setting. We aimed to establish the effect of SRS on survival and cognitive outcomes compared with WBRT in patients with resected brain metastasis.
Methods
In this randomised, controlled, phase 3 trial, adult patients (aged 18 years or older) from 48 institutions in the USA and Canada with one resected brain metastasis and a resection cavity less than 5·0 cm in maximal extent were randomly assigned (1:1) to either postoperative SRS (12–20 Gy single fraction with dose determined by surgical cavity volume) or WBRT (30 Gy in ten daily fractions or 37·5 Gy in 15 daily fractions of 2·5 Gy; fractionation schedule predetermined for all patients at treating centre). We randomised patients using a dynamic allocation strategy with stratification factors of age, duration of extracranial disease control, number of brain metastases, histology, maximal resection cavity diameter, and treatment centre. Patients and investigators were not masked to treatment allocation. The co-primary endpoints were cognitive-deterioration-free survival and overall survival, and analyses were done by intention to treat. We report the final analysis. This trial is registered with ClinicalTrials.gov, number NCT01372774.
Findings
Between Nov 10, 2011, and Nov 16, 2015, 194 patients were enrolled and randomly assigned to SRS (98 patients) or WBRT (96 patients). Median follow-up was 11·1 months (IQR 5·1–18·0). Cognitive-deterioration-free survival was longer in patients assigned to SRS (median 3·7 months [95% CI 3·45–5·06], 93 events) than in patients assigned to WBRT (median 3·0 months [2·86–3·25], 93 events; hazard ratio [HR] 0·47 [95% CI 0·35–0·63]; p<0·0001), and cognitive deterioration at 6 months was less frequent in patients who received SRS than those who received WBRT (28 [52%] of 54 evaluable patients assigned to SRS vs 41 [85%] of 48 evaluable patients assigned to WBRT; difference −33·6% [95% CI −45·3 to −21·8], p<0·00031). Median overall survival was 12·2 months (95% CI 9·7–16·0, 69 deaths) for SRS and 11·6 months (9·9–18·0, 67 deaths) for WBRT (HR 1·07 [95% CI 0·76–1·50]; p=0·70). The most common grade 3 or 4 adverse events reported with a relative frequency greater than 4% were hearing impairment (three [3%] of 93 patients in the SRS group vs eight [9%] of 92 patients in the WBRT group) and cognitive disturbance (three [3%] vs five [5%]). There were no treatment-related deaths.
Interpretation
Decline in cognitive function was more frequent with WBRT than with SRS and there was no difference in overall survival between the treatment groups. After resection of a brain metastasis, SRS radiosurgery should be considered one of the standards of care as a less toxic alternative to WBRT for this patient population.

《壹篇》(与桓兴医讯同步)系主要面向医务人员的公益性头条号,不以营利为目的,不进行任何有偿咨询和服务,不出售任何产品,与ASCO、CSCO等所有专业学会和机构没有任何关系和联系,也不代表任何官方学会发声。
文章图片均来自网络,不做商业用途,若有版权争议请与《壹篇》联系。
坚持点赞、赞赏和转发是一种态度和支持。