引用本文:陈淑佳, 祁胜宾, 孙秀静, 等. 帽状息肉病临床和内镜特征及内镜下切除治疗效果[J]. 中华消化内镜杂志, 2022, 39(10): 838-840. DOI: 10.3760/cma.j.cn321463-20211119-00690.
帽状息肉病临床和内镜特征及内镜下切除治疗效果
陈淑佳1 祁胜宾2 孙秀静1 李鹏1 张澍田1
1首都医科大学附属北京友谊医院消化内科 国家消化系统疾病临床研究中心 北京市消化疾病中心,北京 100050;2石家庄市人民医院消化内科,石家庄 050011
陈淑佳现在石家庄市人民医院消化内科,石家庄 050011
通信作者:陈淑佳,Email:chenshujiadoctor@sina.com
【提要】 为了探讨帽状息肉病的临床、内镜特征,并评价其内镜下切除治疗效果,对2017年6月—2021年2月首都医科大学附属北京友谊医院行内镜黏膜下剥离术(endoscopic submucosal dissection,ESD)或内镜黏膜切除术(endoscopic mucosal resection,EMR)结直肠息肉切除治疗,经术后病理证实为帽状息肉病的14例病例(共56枚息肉)进行了回顾性分析。结果显示:男8例,女6例;年龄14岁~74岁,其中<60岁7例,≥60岁7例;7例(50.0%)伴消化道症状;息肉多发4例,单发10例(71.4%);息肉位于直肠42枚(75.0%),乙状结肠13枚(23.2%),横结肠1枚;山田分型Ⅰ型44枚(78.6%),Ⅱ型3枚,Ⅲ型5枚,Ⅳ型4枚;内镜下息肉表面可见明显白色帽状覆盖物41枚(73.2%)、明显充血发红23枚,其中两者均可见8枚;2例行ESD治疗、12例行EMR治疗,均完全切除,均未出现出血、穿孔、感染等并发症;7例伴消化道症状者术后临床症状均获得缓解;11例(78.6%)随访期间完成肠镜复查,均未见息肉复发。由此可见,帽状息肉病无性别、年龄发病差异,息肉多单发,直肠及乙状结肠多见,形态以山田Ⅰ型为主,表面多有白色帽状覆盖物,患者可无明显消化道症状,内镜下切除治疗安全、有效。
【关键词】 肠息肉; 帽状息肉病; 临床特征; 内镜特征; 内镜黏膜下剥离术; 内镜黏膜切除术
基金项目:河北省医学科学研究课题计划(20210474)
Clinical and endoscopic features and endoscopic treatment efficacy of cap polyposis
Chen Shujia1, Qi Shengbin2, Sun Xiujing1, Li Peng1, Zhang Shutian1
1 Department of Gastroenterology, Beijing Friendship Hospital, Capital Medical University; National Clinical Research Center for Digestive Diseases; Beijing Digestive Disease Center, Beijing 100050, China; 2 Department of Gastroenterology, Shijiazhuang People's Hospital, Shijiazhuang 050011, China
Chen Shujia is working on the Department of Gastroenterology, Shijiazhuang People's Hospital, Shijiazhuang 050011, China
Corresponding author: Chen Shujia, Email: chenshujiadoctor@sina.com
【Summary】 To investigate the clinical and endoscopic characteristics and endoscopic treatment efficacy of cap polyposis, data of 14 patients (56 polyps) who were histologically diagnosed as having cap polyposis after endoscopic submucosal dissection (ESD) or endoscopic mucosal resection (EMR) in Beijing Friendship Hospital from June 2017 to February 2021 was retrospectively analyzed. Of the 14 patients, 8 were males and 6 were females. The age ranged from 14 to 74 years, including 7 cases of <60 years old and 7 cases of ≥60 years old. 7 patients (50.0%) had clinical manifestations. Four cases had multiple polyps and 10 cases (71.4%) had single polyps. There were 42 polyps (75.0%) located in the rectum, 13 (23.2%) in the sigmoid colon and 1 in the transverse colon. According to the classification of Yamada, 44 polyps (78.6%) were type Ⅰ, 3 polyps were type Ⅱ, 5 polyps were type Ⅲ and 4 polyps were type Ⅳ. Under endoscopy, there were 41 polyps (73.2%) with obvious white cap-like coverings on the surface and 23 polyps with obvious hyperemia and redness on the mucosa, 8 of which were both visible. Two cases were treated with ESD and 12 cases were treated with EMR, all of which were completely excised. No bleeding, perforation, infection or other complications occurred during and after operation. The clinical symptoms of 7 patients were relieved. During the follow-up period, 11 cases (78.6%) completed colonoscopy, and no polyp recurrence was found. In conclusion, there is no gender or age difference in patients of cap polyposis. It is usually single and located in the rectum and sigmoid colon with Yamada type Ⅰ. The surface of lesions is mostly covered with white cap. Patients may have no obvious clinical symptoms. Treatment of ESD and EMR is safe and effective for cap polyposis.
【Key words】 Intestinal polyps; Cap polyposis; Clinical features; Endoscopic features; Endoscopic submucosal dissection; Endoscopic mucosal resection
Fund program: Medical Science Research Project of Hebei Province (20210474)
帽状息肉病是一种少见的肠道炎症性疾病,首次报道于1985年,因息肉表面覆盖一层炎性肉芽组织的“帽”而得名,好发于远端结肠及直肠,患者可以出现腹泻、便血、直肠黏膜脱垂等临床表现[1‑5]。目前国内关于帽状息肉病内镜诊治的相关报道较少,本研究对首都医科大学附属北京友谊医院消化内镜中心治疗的帽状息肉病病例进行了回顾性分析,旨在为临床提供参考。
一、资料与方法
1.病例资料:2017年6月—2021年2月,因结直肠息肉在首都医科大学附属北京友谊医院行ESD或EMR治疗,经术后病理证实为帽状息肉病的患者共14例(56枚息肉),占首都医科大学附属北京友谊医院同期因结直肠息肉行EMR或ESD治疗患者总数的1.5‰(14/9125)。以上14例患者术前常规检查已除外治疗禁忌,治疗前均已签署知情同意书。
2.手术器材:日本Olympus公司GIF‑Q260J型、CF‑H290Z型内镜,黏膜注射针,Dual刀,IT刀,圈套器,凝血钳,甘油果糖,透明质酸钠,亚甲蓝,肾上腺素注射液,生理盐水注射液,钛夹,CO2气泵,注水泵,透明帽等。
3.内镜治疗
(1)ESD:①确定病变范围与深度:了解病灶的部位、大小和形态,结合染色和放大内镜检查确定病灶的范围、性质和浸润深度;②病灶边缘标记:明确病灶边界,距病灶边缘3~5 mm处进行电凝标记;③黏膜下注射:于病灶边缘标记点外侧进行多点黏膜下注射,将病灶抬起,与肌层分离,有利于ESD完整地切除病灶,而不容易损伤固有肌层,减少穿孔和出血等并发症的发生;④切开:沿标记点外侧缘切开病变周围部分黏膜,再深入切开黏膜下层,切开周围全部黏膜;⑤黏膜下剥离:在进行剥离前判断病灶抬举情况,必要时需反复黏膜下注射维持病灶充分抬举,将黏膜与固有肌层完全剥离,完整切除病灶;⑥创面处理:对剥离后创面上所有的血管进行预防性止血处理,渗血部位使用止血钳、氩离子凝固术,对局部剥离较深或肌层有裂隙者使用钛夹夹闭。术后常规禁食24~48 h,存在感染高危因素者予抗菌药物。

1A:山田Ⅰ型;1B:山田Ⅱ型
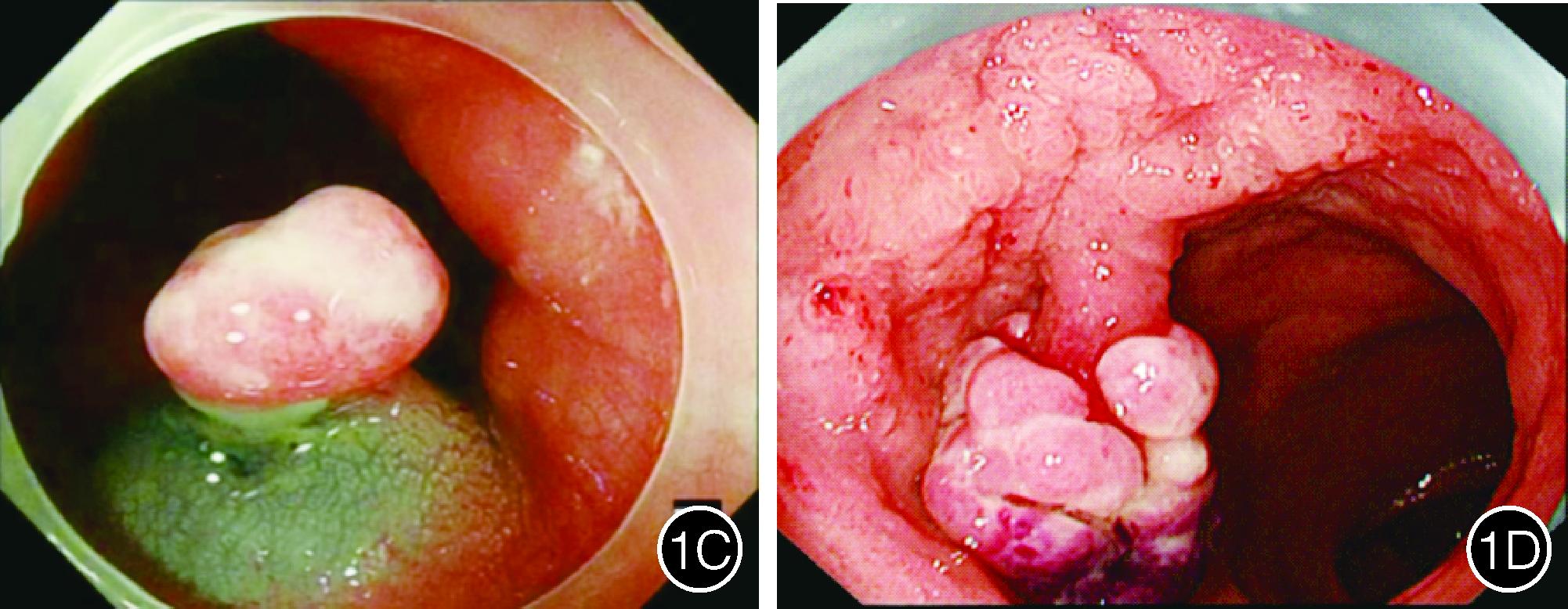
1C:山田Ⅲ型;1D:山田Ⅳ型
图1 帽状息肉的白光内镜下形态;
(2)EMR:①应用生理盐水及亚甲蓝注射液于息肉基底部进行黏膜下注射;②抬举征阳性后应用圈套器完整切除病变;③依据创面情况予凝血钳、氩离子凝固术、钛夹等处理。术后常规禁食24 h。
4.组织学评价:切除标本放入10%的甲醛溶液中固定,测量病变大小,如病变为ESD切除标本,除测量切除黏膜大小外还需测量黏膜上息肉大小,每隔2 mm平行切开标本,按顺序竖立包埋,切片厚度4~5 μm,染色后显微镜下观察。
二、结果
1.临床特点:男8例,女6例。年龄14~74岁,其中<60岁7例,≥60岁7例。常规结肠镜检查中发现者5例;因肛周不适发现肛周肿物2例;其余7例(50.0%)伴有消化道症状,包括便血4例、脱肛伴便血1例、腹泻2例。7例既往体健;2例有痔疮病史;1例有直肠癌手术史;1例有结肠息肉病史;1例有直肠炎病史;1例既往行13C呼气试验结果阳性,已口服药物根除幽门螺旋杆菌,复查呼气试验结果阴性;1例行13C呼气试验结果阳性,提示幽门螺旋杆菌现症感染。
2.内镜特点:多发息肉4例,单发10例(71.4%);息肉位于直肠42枚(75.0%),乙状结肠13枚(23.2%),横结肠1枚;山田分型Ⅰ型44枚(78.6%),Ⅱ型3枚,Ⅲ型5枚,Ⅳ型4枚(图1);息肉长径0.4~2.8 cm,其中≥1.0 cm 15枚、<1.0 cm 41枚(73.2%);内镜下息肉表面可见明显白色帽状覆盖物41枚(73.2%)、明显充血发红23枚,其中两者均可见8枚。
3.治疗效果:2例行ESD治疗,均整块切除,术后切缘干净;其余12例行EMR治疗,均完全切除。14例均未出现出血、穿孔、感染等治疗相关并发症。术前有消化道症状的7例,术后临床症状缓解。2例ESD治疗者和2例EMR治疗者1年后在北京友谊医院复查肠镜,均未见息肉复发;7例EMR治疗者1年后在当地医院复查肠镜,均未见息肉复发;3例未能成功随访。
讨论
帽状息肉病是一种少见的肠道炎症性疾病,确切发病率尚无文献报道。本研究统计了4年来在北京友谊医院因结直肠息肉行EMR或ESD治疗的总例数以及切除后病理报告为帽状息肉病的例数,发现帽状息肉病占比仅为1.5‰。本组病例中,男8例、女6例,年龄<60岁7例、≥60岁7例,提示本病可能无明显性别及年龄发病差异。本研究中,仅7例(50.0%)伴有消化道症状,包括便血4例、脱肛伴便血1例、腹泻2例,提示本病可无明显临床表现。以往多个文献报道本病与幽门螺旋杆菌感染相关[6‑8],本组中有1例有幽门螺旋杆菌既往感染,另有1例有幽门螺旋杆菌现症感染。杨凯茜等[9]报道直肠炎症性帽状息肉病多发生在肛管直肠黏膜脱垂的基础上,本组中1例有脱肛临床表现,可能是由于肛管直肠黏膜和黏膜下层组织脱垂后造成一过性缺血引起的继发改变。Aggarwal等[10]报道了1例因反复发作帽状息肉病行左半结肠切除术时发现广泛血管畸形的病例,推测这也可能是帽状息肉病的一个病因。另外,也有报道称感染、肠道菌群失调也可能是帽状息肉病的发病因素[3, 11]。
本研究中,单发息肉占71.4%,直肠息肉占75.0%、乙状结肠息肉占23.2%,山田Ⅰ型息肉占78.6%,息肉长径<1 cm占73.2%,内镜下息肉表面白色帽状覆盖物发现率为73.2%,提示帽状息肉病息肉单发者居多,直肠及乙状结肠多见,形态以山田Ⅰ型为主,表面多有白色帽状覆盖物。
Inagaki等[8]报道帽状息肉病患者可通过根除幽门螺杆菌达到症状缓解和息肉消失,少部分可通过5-氨基水杨酸、类固醇、甲硝唑、英夫利昔单抗等药物治疗好转[12],外科手术切除部分肠段也可用来治疗复发或多发帽状息肉病[1‑2],另外也可行内镜下治疗[13‑14]。本研究中,1例有慢性腹泻临床表现,13C呼气试验提示幽门螺旋杆菌现症感染,但在根除细菌后症状并未见明显好转,之后在行息肉内镜下切除后,患者腹泻症状得到好转,这与Murata等[15]的报道极为相似。本研究中,具有便血等消化道表现的7例患者,经息肉内镜下治疗后症状均有好转,提示帽状息肉病患者行EMR或ESD切除息肉治疗有效。
综上,本研究结果初步显示,帽状息肉病无性别、年龄发病差异,息肉多单发,直肠及乙状结肠多见,形态以山田Ⅰ型为主,表面多有白色帽状覆盖物,患者可无明显消化道症状,内镜下切除治疗安全、有效。但本研究为单中心、小样本的回顾性分析,且随访时间有限,存在局限和不足之处,因此今后仍需多中心、大样本的前瞻性研究来提供更为可靠的数据,以便制定我国帽状息肉病的诊治策略。
利益冲突 所有作者声明不存在利益冲突
作者贡献声明
陈淑佳:设计研究,实施研究,文章撰写;祁胜宾:数据采集及分析;孙秀静:设计研究,材料支持;李鹏:技术支持及指导;张澍田:行政支持及技术指导
参考文献
[1] Ng KH, Mathur P, Kumarasinghe MP, et al. Cap polyposis: further experience and review[J]. Dis Colon Rectum, 2004,47(7):1208-1215. DOI: 10.1007/s10350-004-0561-8.
[2] Tamura K, Matsuda K, Yokoyama S, et al. Successful laparoscopic resection for cap polyposis: case report, literature review[J]. Surg Case Rep, 2018,4(1):69. DOI: 10.1186/s40792-018-0476-6.
[3] Okamoto K, Watanabe T, Komeda Y, et al. Dysbiosis-associated polyposis of the colon-cap polyposis[J]. Front Immunol, 2018,9:918. DOI: 10.3389/fimmu.2018.00918.
[4] Esaki M, Matsumoto T, Kobayashi H, et al. Cap polyposis of the colon and rectum: an analysis of endoscopic findings[J]. Endoscopy, 2001,33(3):262-266. DOI: 10.1055/s-2001-12797.
[5] Peny MO, Noel JC, Haot J, et al. Cap polyposis: a rare syndrome[J]. Gastroenterol Clin Biol, 1998,22(3):349-352.
[6] Nishiyama M, Maeda K, Aoyagi K, et al. Cap polyposis and Helicobacter pylori[J]. Nihon Rinsho, 2005,63 Suppl 11:328-330.
[7] Takeshima F, Senoo T, Matsushima K, et al. Successful management of cap polyposis with eradication of Helicobacter pylori relapsing 15 years after remission on steroid therapy[J]. Intern Med, 2012,51(4):435-439. DOI: 10.2169/internalmedicine.51.6376.
[8] Inagaki Y, Shimomura T, Suzuki T, et al. A case of cap polyposis achieving complete remission by Helicobacter pylori eradication therapy[J]. Nihon Shokakibyo Gakkai Zasshi, 2021,118(2):183-187. DOI: 10.11405/nisshoshi.118.183.
[9] 杨凯茜, 黄秀江, 李笑云. 直肠炎症性帽状息肉病二例[J].中华消化内镜杂志,2021,38(2):159-160. DOI: 10.3760/cma.j.cn321463-20200429-00340.
[10] Aggarwal A, Lang A, Krigman HR, et al. Vascular malformation and cap polyposis: a new insight into pathophysiology or fortuitous association?[J]. Fetal Pediatr Pathol, 2022,41(4):670-676. DOI: 10.1080/15513815. 2021.1913537.
[11] da Cunha Araújo RN, Castanheira A, Silva A. Unusual colon polyps. Diagnosis: cap polyposis[J]. Gastroenterology, 2011,141(4):e1-2. DOI: 10.1053/j.gastro.2010.07.066.
[12] 贾燕, 杨浪, 陆晓娟, 等. 第536例腹泻—直肠多发隆起伴糜烂—帽状息肉病[J].中华医学杂志,2021,101(16):1186-1188. DOI: 10.3760/cma.j.cn112137-20201226-03475.
[13] Anuchapreeda S, Phengsuthi P, Aumpansub P, et al. Polypectomy for recurrent inflammatory cap polyposis combined with argon plasma coagulation[J]. ACG Case Rep J, 2018,5:e35. DOI: 10.14309/crj.2018.35.
[14] Monsalve Alonso S, Miranda García P, Santander Vaquero C. Endoscopic mucosal resection for cap poliposis treatment[J]. Rev Esp Enferm Dig, 2020,112(2):155. DOI: 10.17235/reed.2020.6537/2019.
[15] Murata M, Sugimoto M, Ban H, et al. Cap polyposis refractory to Helicobacter pylori eradication treated with endoscopic submucosal dissection[J]. World J Gastrointest Endosc, 2017,9(10):529-534. DOI: 10.4253/wjge.v9.i10.529.